New research led by the Daffodil Centre’s Professor Anne Cust has provided evidence that routine skin checks by a health professional, coupled with checking your own skin, are vital in saving lives from melanoma – the most deadly form of skin cancer.
Australia has the highest melanoma rates in the world, with one person dying every 6 hours from the disease. Melanoma is also the most common cancer in 20 to 39-year-olds.
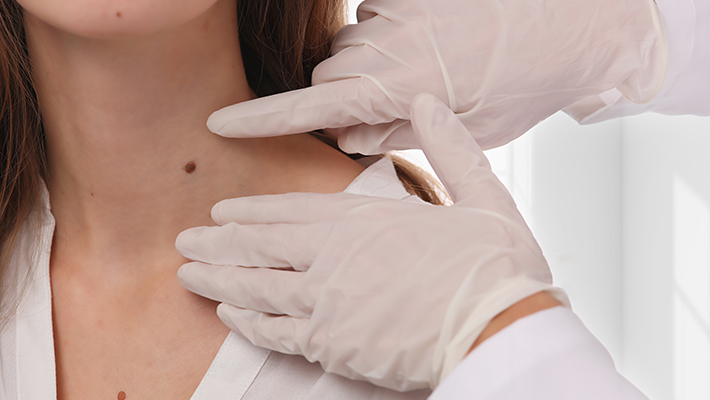
The first sign of melanoma is often a new or changing spot or mole on the skin. However, melanoma can vary greatly in its appearance and many subtle clues can only be detected by a trained healthcare professional using a magnifying tool, known as a dermatoscope, to check the skin.
The research, published in JAMA Dermatology, found that in a group of 2,452 patients diagnosed with melanoma, slower-growing melanomas were more likely to be detected at a routine skin check and be thinner, whereas faster-growing melanomas were more likely to be patient-detected and thicker. It was estimated that patients whose melanoma was detected by their doctor during a routine skin check were 32% less likely to die from melanoma compared to patients who identified their own melanoma, although there was uncertainty around this estimate and a large randomised controlled trial is needed to provide definitive evidence.
The study also found that melanomas easily detected using the ABCDE rule were more likely to be detected by the patients (70%), whereas atypical ones were more often detected by a doctor during a routine skin check.
Current Australian guidelines recommend that individuals at very high risk of melanoma receive full skin examinations every 6 months. However, melanoma screening programs for the general population are not currently undertaken in Australia because of inadequate evidence that melanoma screening ultimately saves lives, uncertainty about overdiagnosis and unnecessary biopsy, and limited evidence that it is cost effective.
In the last decade there has been renewed interest in melanoma screening, driven by the changing landscape of melanoma care.
“We found that melanoma detection during a routine skin check was associated with lower risk of dying from any cause, but it was not statistically significant for melanoma-specific mortality,” said Prof Cust.
“Based on our early findings, the cost-effectiveness of a population melanoma screening program should be re-assessed.”
Professor Cust is a Faculty member of the Melanoma Institute Australia, where she co-leads the ‘Prevention, risk and clinical detection of melanoma’ research theme and Chairs the Research Committee. This study was funded by the National Health and Medical Research Council, Cancer Institute NSW and Melanoma Institute Australia.